.avif)
From Scribe to Final Note
A360 Notes receives structured and cleaned consult data from Scribe and organizes it into clinical record sections. The result is a clear, editable draft that reduces missed details and eliminates manual rewriting.
Uses Scribe's structured output
Organizes into note sections
Creates an editable draft
Produces a consistent final note
Practice-Standard Language, Every Time
Notes applies practice conventions so documentation matches how your clinic actually documents care. It uses standardized language and correct service naming to keep notes consistent provider to provider.
Applies practice conventions
Uses preferred terminology
Standardizes service names
Improves provider consistency
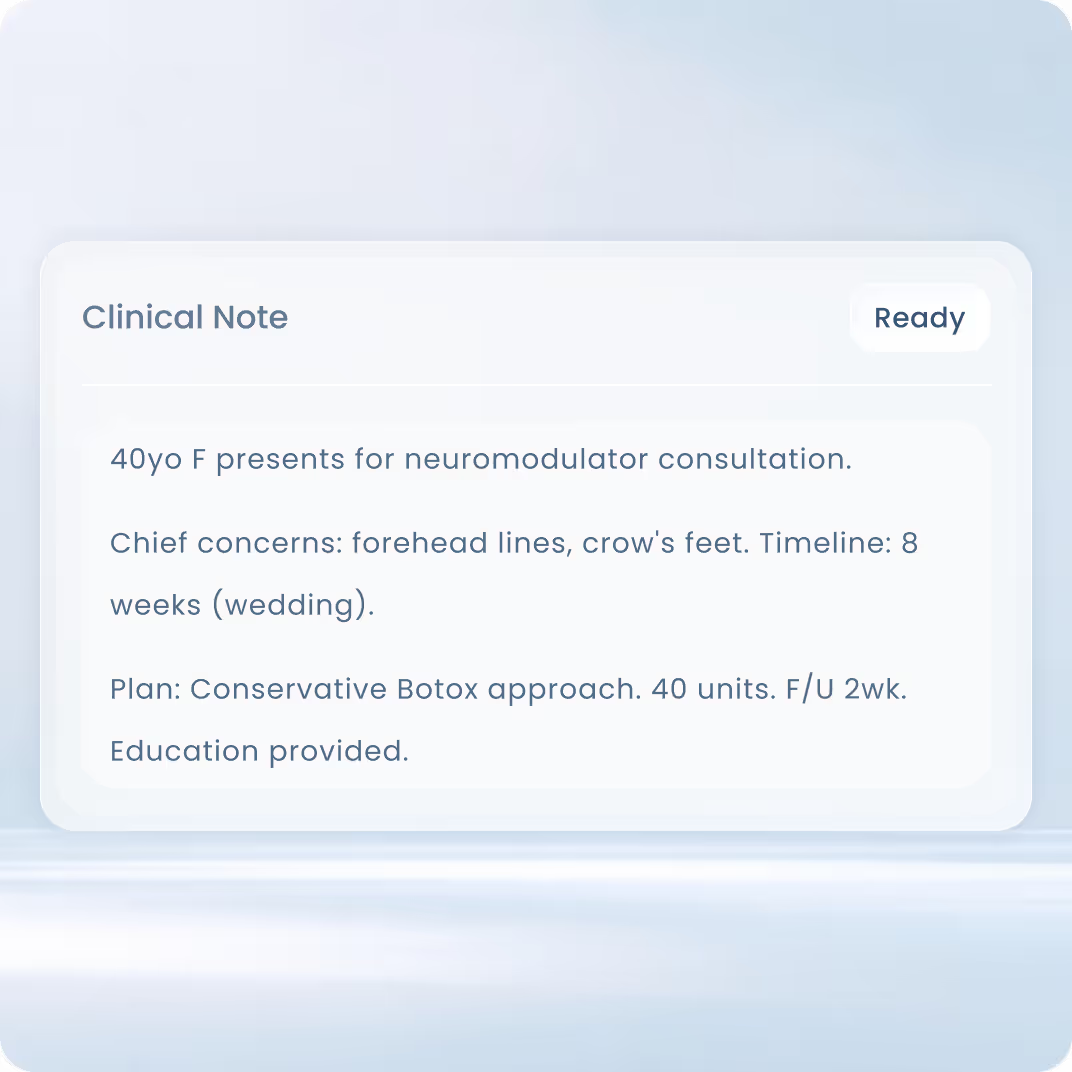

Provider-Controlled and EMR-Ready
The provider stays in control. Notes produces a structured document that can be edited, refined, expanded, and signed off—then finalized for the patient chart or EMR.
Provider reviews and edits
Prevents missing details
Finalize and sign off
Copy, export, or sync*
Specific documentation features that support operations and compliance
Structured Note Draft
Turns Scribe output into a clean, organized clinical note draft.
No New Clinical Content
Does not invent, rewrite, or make treatment decisions.
Practice Conventions Applied
Uses preferred terminology, formatting, and standardized phrasing.
Editable Provider Workflow
Provider can edit, refine, expand, and sign off.
Section-Level Organization
Places information into common documentation sections.
EMR-Ready Output
Final note prepared for chart storage; copy/export/sync based on integration.
Your Questions Answered
What is A360 Notes?
A360 Notes transforms consultation conversations into structured clinical documentation aligned with practice standards.
How are notes created?
A360 listens to consultations, identifies clinically relevant information, and organizes it into structured notes.
How much control does the practice have over note structure?
Practices define required sections, structure, and language to ensure consistency.
Can practices customize the language used in notes?
Yes. Preferred terminology and phrasing can be specified and applied automatically.
What happens when providers edit notes?
Edits are treated as feedback and improve future accuracy.
How does A360 handle different visit types?
It recognizes visit types and adjusts documentation accordingly.
Does A360 Notes replace provider responsibility?
No. Providers review and approve all notes; clinical responsibility remains with them.
Can A360 Notes be used without other modules?
Yes. It can be used independently or alongside other A360 modules.
How does A360 Notes improve documentation quality?
By standardizing structure and language, it reduces variability and missed details.
Why adopt A360 Notes instead of templates or dictation?
Templates are static and dictation is time-consuming. A360 Notes adapts and improves over time.
Ready to turn consults into revenue?






